Ozempic and Wegovy (semaglutide) are widely popular right now.
When weight loss drugs hit the market, the make a big splash but Semaglutide is making massive waves in the weight loss arena. And, it has quickly evolved into a vanity drug despite being a medical drug.
What is Semaglutide?
Semaglutide is a peptide that helps regulate how our bodies manage sugar and metabolism.
As with most weight loss drugs, the news is on fire touting the benefits and ignoring the potential issues associated with their use. As a side note, Semaglutide is intended to work as long as you take it. What happens after side effects cause people to discontinue using it? Weight gain. Frustration.
Curious about the possible side effects? Check out this partial list:
- Nausea
- Vomiting
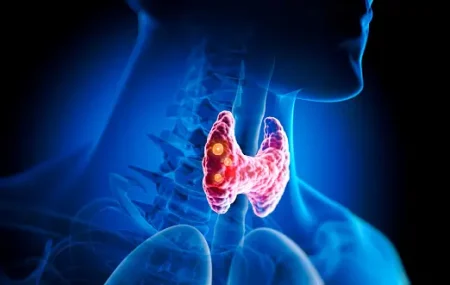
- Increased risk of thyroid tumors
- Increased risk of pancreatitis
- Depression
- Diarrhea with urgency
- Constipation
- Bloating and Gas
- Headaches
- Dizziness
- Fatigue
- Loss of appetite
- Abdominal pain
- Heartburn
- Yellow eyes and skin
- Hair loss
There is also a VERY long list of medications that should be avoided if you use Semaglutide. If you are a user of Semaglutide or are considering using it, I highly recommend not skipping the fine print.
The human body actually has it’s own built-in mechanisms that these drugs mimic, without the side effects.
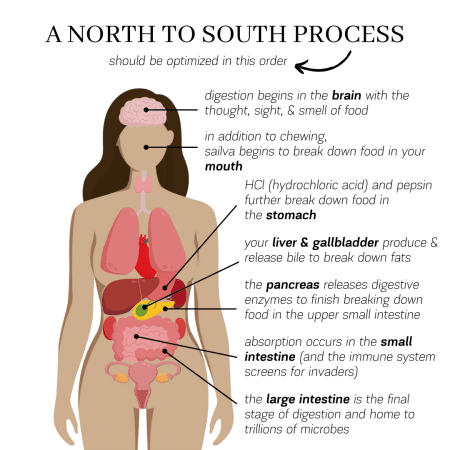
Semaglutide mimics a peptide that is naturally made in the body called glucagon-like-peptide-1 (GLP-1). GLP-1 is released in the gastrointestinal tract when we eat. This prompts the release of insulin to regulate our blood sugar levels. GLP-1 also communicates with the brain to help reduce appetite when energy is not needed and creates a feeling of fullness or satiety.
Turns out, there are bacterial species in our microbiome (the collection of bacteria that reside in our digestive tract) that take food we don’t fully digest (like fiber!) and transform it into GLP-1 (and other molecules like PYY that helps regulate blood sugar) that control appetite and metabolism.
Modern food processing negatively impacts our natural ability to produce adequate amounts of GLP-1 and PYY by removing many of the beneficial molecules like fiber and polyphenols that feed the bacterial populations responsible for these important processes. The more we move towards a diet heavy in processed foods, the less healthy our microbiomes become and in turn, the less healthy we become.
While these weight loss therapies seem like magic bullets, they are not without negative effects on the body as a whole.
We recommend taking a more personalized approach to weight management that includes a look at each individuals microbiome, comprehensive blood work, dietary intake, stress levels, sleep cycles, body movement and of course, food relationship.
The greatest results do, most often, come with looking at each person as a unique individual and creating a balanced approach that is sustainable.





 #2 – This might be a tough pill to swallow for some since there are so many convenient options on every corner but, if you can mostly make your own food, you will be well rewarded. Cooking at home has a lot of advantages including knowing every single ingredient you will be consuming and knowing that your food is not combined with countless chemicals. Convenient, fast foods usually use low grade oils that can contribute to inflammation, dyes that our bodies are not capable of breaking down and WAY too much sugar – heck they even put sugar in soup!
#2 – This might be a tough pill to swallow for some since there are so many convenient options on every corner but, if you can mostly make your own food, you will be well rewarded. Cooking at home has a lot of advantages including knowing every single ingredient you will be consuming and knowing that your food is not combined with countless chemicals. Convenient, fast foods usually use low grade oils that can contribute to inflammation, dyes that our bodies are not capable of breaking down and WAY too much sugar – heck they even put sugar in soup! #3 – Next, remember these two acronyms and don’t get bogged down with all the heavy details of weighing and measuring food or calorie counting that can feel so overwhelming:
#3 – Next, remember these two acronyms and don’t get bogged down with all the heavy details of weighing and measuring food or calorie counting that can feel so overwhelming: #4 – Lastly, digestion works best when we are in a relaxed state so try eating intentionally. This really means to simply slow down, take a few deep breaths prior to eating, relax and clear your mind of all the worries of your day.
#4 – Lastly, digestion works best when we are in a relaxed state so try eating intentionally. This really means to simply slow down, take a few deep breaths prior to eating, relax and clear your mind of all the worries of your day. If you’re in pursuit of achieving better health, you should be tracking – where you’re at, where you want to be and what’s standing in your way.
If you’re in pursuit of achieving better health, you should be tracking – where you’re at, where you want to be and what’s standing in your way. The history of sugar is a fascinating but troubling story. If you have time to do a little research, you might agree. We won’t delve into the depths of that today but I do want to speak to what happens when we consume sugar and ways you can reduce your cravings for sugar in a sustainable way for the benefit of longevity and better health.
The history of sugar is a fascinating but troubling story. If you have time to do a little research, you might agree. We won’t delve into the depths of that today but I do want to speak to what happens when we consume sugar and ways you can reduce your cravings for sugar in a sustainable way for the benefit of longevity and better health.  One of my favorite quotes is “Those with chronic illness aren’t faking being sick. They are actually faking being well.”
One of my favorite quotes is “Those with chronic illness aren’t faking being sick. They are actually faking being well.” 
